
Breast implant safety
Family psychology
Elderly couple issues
Depression treatment
Couple counselling
Stress issues
Family psychology
Elderly couple issues
Depression treatment
Couple counselling
Stress issues
HAVE A QUESTION ABOUT THIS?

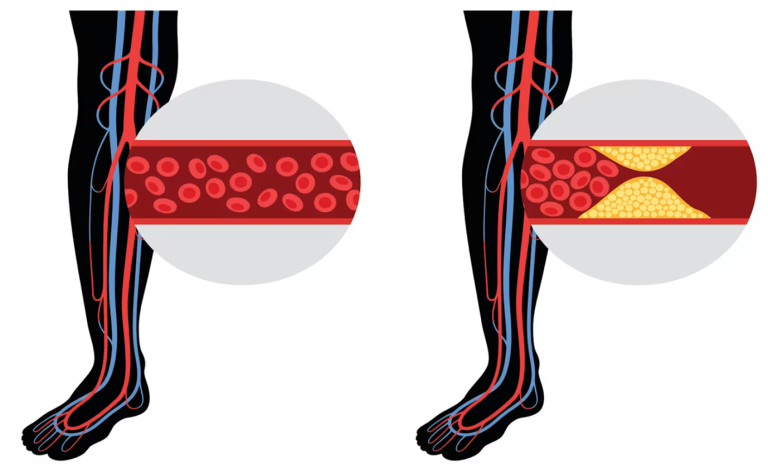
Peripheral Arterial Disease (blocked arteries)
Peripheral artery disease (PAD) happens when the arteries that supply blood to your arms or legs become narrowed. In most cases, it affects your legs. When this happens, your muscles do not receive enough blood during activity, which can cause pain and other symptoms.
PAD is usually a sign of atherosclerosis — a build-up of fatty deposits (plaque) inside your arteries. This build-up reduces blood flow and can also affect the heart and brain.
Symptoms
You may not notice any symptoms at first, or they may be mild. Common symptoms include:
- Pain in your legs when walking (known as claudication).
- Cramping or aching in your calves, thighs, hips, or buttocks during activity that settles with rest.
- Coldness in one lower leg or foot compared with the other side.
- Numbness or weakness in your legs.
As PAD progresses, you may experience:
- Pain that becomes more severe.
- Pain that wakes you at night.
- Pain at rest, especially when lying flat.
- Difficulty walking even short distances.
Other possible signs include:
- Shiny skin on your legs.
- Changes in skin colour.
- Hair loss or slower hair growth on your legs.
- Sores on your toes, feet, or legs that do not heal.
When to Seek Medical Advice
If you have leg or arm pain during activity, pain at rest, or any non-healing wounds on your feet or legs, you should arrange a medical assessment. Early diagnosis can prevent serious complications.
Risk Factors
You are at higher risk of PAD if you:
- Smoke or have smoked.
- Have diabetes.
- Have high blood pressure.
- Have high cholesterol.
- Are overweight.
- Have a family history of heart disease, stroke, or PAD.
- Are over 65, or over 50 with other cardiovascular risk factors.
Possible Complications
If left untreated, PAD can lead to:
Critical limb ischaemia
This is a severe reduction in blood flow. You may develop persistent rest pain, non-healing ulcers, or tissue damage.
Heart attack or stroke
PAD is a sign of widespread atherosclerosis, which increases your risk of cardiovascular events.
How You Can Reduce Your Risk
You can lower your risk of developing PAD — or prevent it from getting worse — by making lifestyle changes:
- Stop smoking.
- Eat a healthy diet low in sugars and saturated fats.
- Exercise regularly (after discussing a safe plan with your clinician).
- Maintain a healthy weight.
- Control your blood pressure.
- Manage your cholesterol levels.
- Keep your diabetes well controlled.
- Improve sleep and reduce stress.
If you are concerned about symptoms of peripheral artery disease, early assessment and treatment can significantly improve outcomes and protect your long-term vascular health.
Diagnosis of Peripheral Artery Disease (PAD)
If PAD is suspected, you will be asked about your symptoms and medical history, and your circulation will be examined. The pulse in your feet or legs may be weak or absent.
Tests You May Need
Blood tests
These check for risk factors such as high cholesterol and high blood sugar.
Ankle–Brachial Index (ABI)
This is a simple, painless test that compares the blood pressure in your ankle with the blood pressure in your arm. A lower ankle reading suggests reduced blood flow to your legs.
Doppler Ultrasound
A Doppler scan can identify narrowed or blocked arteries in your legs.
CT Angiogram
A contrast dye is injected into your bloodstream to make your arteries visible on imaging. This helps identify the exact location and severity of blockages.
Treatment of Peripheral Artery Disease (PAD)
The aims of treatment are to:
- Relieve your symptoms (such as leg pain).
- Improve your walking distance and quality of life.
- Reduce your risk of heart attack, stroke, and other vascular complications.
Treatment may include lifestyle changes, medication, and in some cases, procedures or surgery.
Lifestyle Changes
If your PAD is in its early stages, lifestyle measures can significantly improve symptoms and slow progression.
You should:
- Stop smoking completely.
- Exercise regularly (ideally supervised exercise therapy).
- Follow a heart-healthy diet.
- Maintain a healthy weight..
Medications
You may need medication to control symptoms and reduce cardiovascular risk.
Statins
These lower LDL (“bad”) cholesterol, reduce plaque build-up, and decrease the risk of heart attack and stroke.
Blood pressure medication
Controlling blood pressure prevents further arterial damage and improves circulation.
Diabetes treatment
If you have diabetes, tight blood sugar control reduces complications and disease progression.
Blood thinner medication
Aspirin or clopidogrel may be prescribed to reduce the risk of blood clots.
Procedures and Surgery
If symptoms are severe or affect your lifestyle and medical therapy are insufficient, intervention may be required.
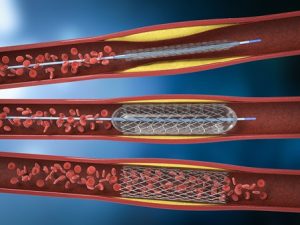
Key hole Surgery (Angioplasty and Stenting)
A small balloon is inserted into the narrowed artery and inflated to widen it. A stent (metal mesh tube) may be placed to keep the artery open and improve blood flow.
Bypass Surgery
If the blockage is extensive, a new route for blood flow can be created using one of your own veins or a synthetic graft. This bypasses the blocked segment and restores circulation.
Foot Care
Good foot care is essential, particularly if you have PAD and diabetes. Reduced blood flow makes wounds slower to heal and increases the risk of infection.
You should:
- Wash your feet daily and dry them thoroughly.
- Use moisturiser to prevent cracked skin (avoid between the toes).
- Wear well-fitting shoes and clean, dry socks.
- Treat fungal infections promptly.
- Trim toenails carefully.
- Inspect your feet daily for cuts, blisters, or sores.
- Seek medical advice immediately if you notice any wounds.
Early diagnosis and appropriate treatment significantly reduce the risk of limb complications and cardiovascular events.

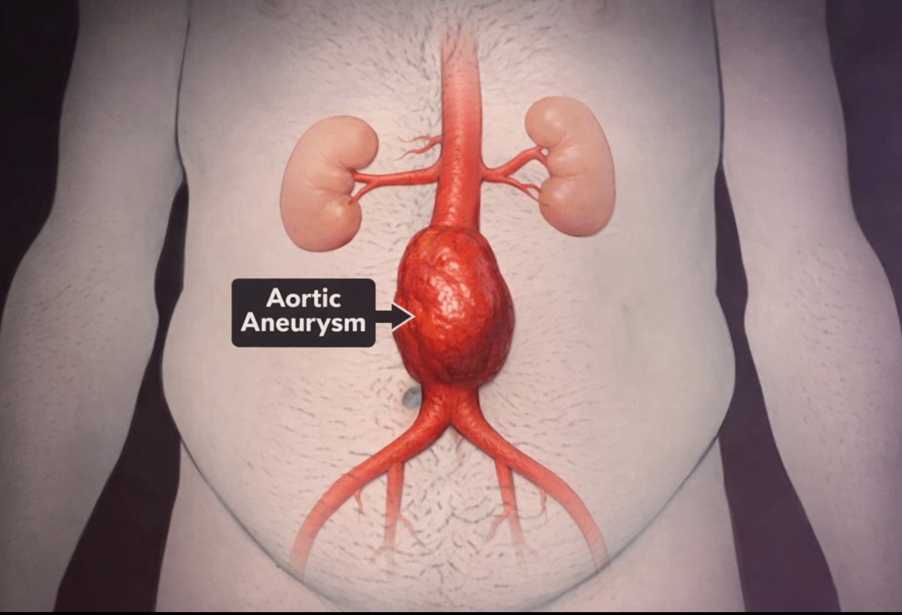
Abdominal Aortic Aneurysm (AAA)
An abdominal aortic aneurysm (AAA) happens when the lower part of your body’s main artery — the aorta — becomes enlarged. The aorta runs from your heart, through your chest, and into your abdomen.
AAAs usually grow slowly. In most cases, you will not notice any symptoms, which is why they are often discovered incidentally or through screening. Some aneurysms remain small and stable. Others enlarge over time, sometimes quickly. If an aneurysm ruptures, it can cause life-threatening internal bleeding.
What symptoms might you notice?
If your aneurysm is enlarging, you may experience:
- Deep, constant pain in your abdomen or the side of your abdomen
- Persistent back pain
- A throbbing or pulsing sensation near your belly button
If an aneurysm ruptures, symptoms can include:
- Sudden, severe and persistent abdominal or back pain (often described as tearing or ripping)
- Dizziness or fainting due to low blood pressure
- A rapid pulse
A ruptured aneurysm is a medical emergency and requires immediate treatment.
What increases your risk?
You are more likely to develop an abdominal aortic aneurysm if you:
- Smoke or have smoked– this is the strongest risk factor. Smoking weakens the aortic wall and increases the risk of growth and rupture.
- Are aged 65 or older
- Are male
- Have a family history of abdominal aortic aneurysm
- Have had another aneurysm (for example in the chest or behind the knee)
- Have high blood pressure or other cardiovascular disease
How can you reduce your risk?
You can lower your risk of developing or worsening an aneurysm by:
- Stopping smoking and avoiding second-hand smoke
- Controlling your blood pressure and cholesterol
- Eating a balanced diet rich in fruit, vegetables, whole grains and lean protein
- Reducing salt and unhealthy fats
- Exercising regularly (aim for at least 150 minutes of moderate activity per week, if appropriate for you)
NHS AAA Screening Programme (NAAASP)
If you are a man aged 65 or over in England, you will automatically be invited for a free abdominal aortic aneurysm screening scan through the NHS Abdominal Aortic Aneurysm Screening Programme.
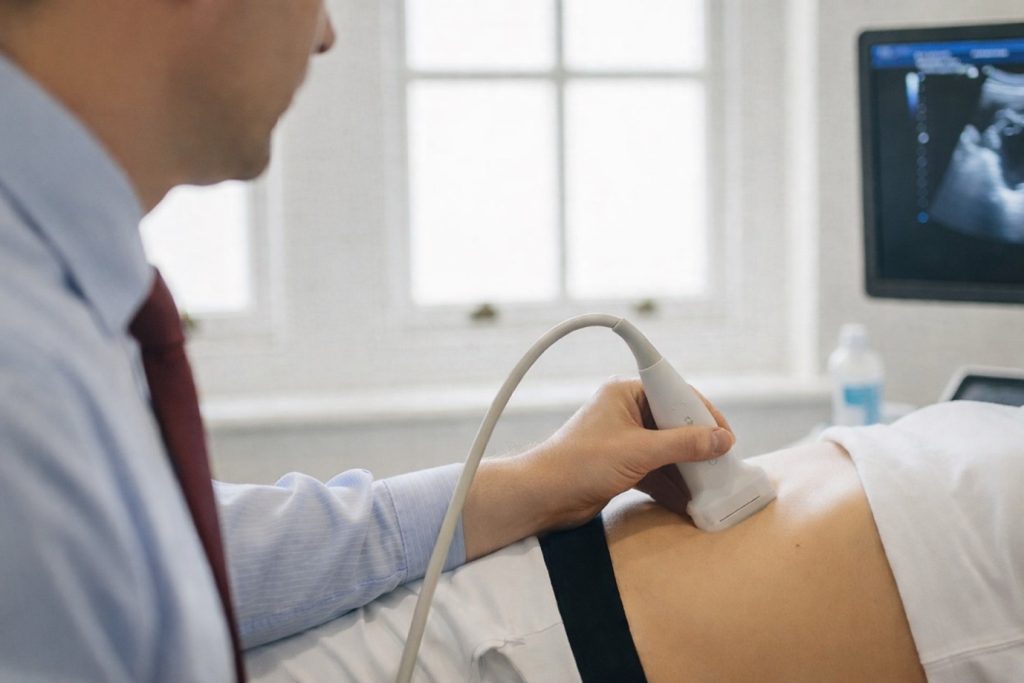
This involves a quick, painless ultrasound scan of your abdomen to check the size of your aorta.
How is an AAA diagnosed?
An abdominal aortic aneurysm is often found during a scan performed for another reason.
To confirm the diagnosis, you may have:
- Abdominal ultrasound– the most common test, using sound waves to measure the size of your aorta
- CT scan– provides detailed images and precise measurements
- MRI scan– sometimes used for further assessment
CT and MRI scans may involve contrast dye to show your blood vessels more clearly.
How is an AAA managed?
The aim of treatment is to prevent rupture. Your management depends mainly on the size of the aneurysm and how quickly it is growing.
1. Monitoring (Watchful Waiting)
If your aneurysm is small and not causing symptoms, you may not need immediate intervention.
You will have:
- Regular ultrasound scans to monitor growth
- Blood pressure control
- Cardiovascular risk optimisation
Small aneurysms are typically monitored at regular intervals, often every 6–12 months depending on size.
2. Aneurysm Repair
Intervention is usually recommended if:
- Your aneurysm is around 5.5 cm or larger
- It is growing rapidly
- You have symptoms
- There are signs of leakage
Your treatment options include:
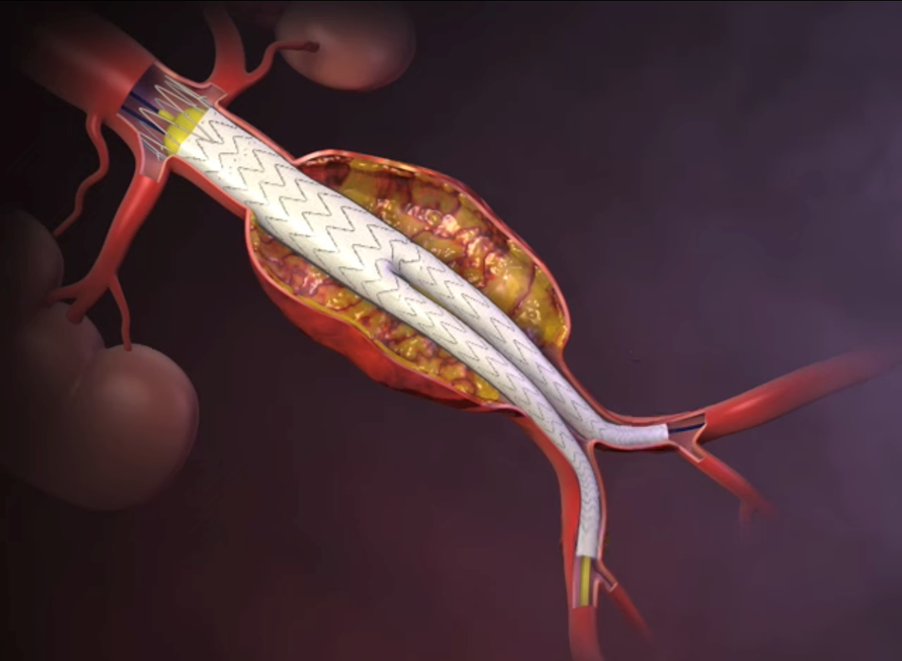
Endovascular Aneurysm Repair (EVAR)
This is a minimally invasive procedure performed through the arteries in your groin. A stent graft is placed inside your aorta to reinforce the weakened section and exclude the aneurysm from blood flow.
Advantages:
- Smaller incisions
- Shorter hospital stay
- Faster recovery
You will require lifelong imaging follow-up to ensure the graft remains secure and there is no leakage.
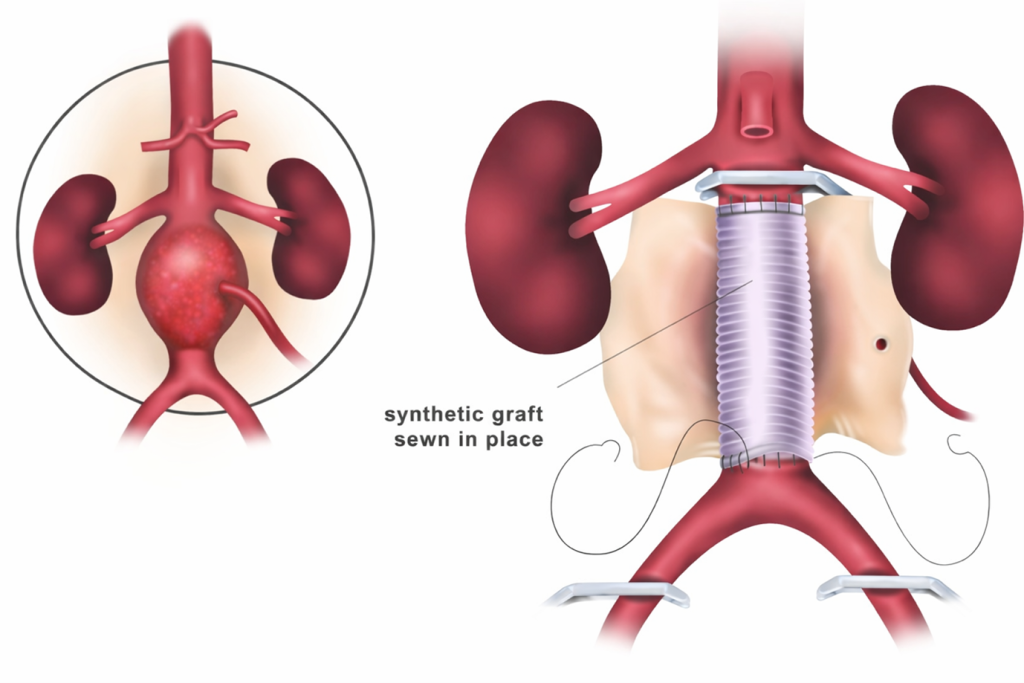
Open Surgical Repair
This involves replacing the weakened section of your aorta with a surgical graft through an abdominal incision.
More invasive and recovery takes longer than EVAR, but we think it is more durable.
Possible Complications
If left untreated, an abdominal aortic aneurysm can lead to:
- Rupture, causing life-threatening bleeding
- Aortic dissection(a tear in the aortic wall)
- Blood clot formation, which can block blood flow to your legs, kidneys or abdominal organs
When should you seek urgent medical help?
Seek emergency medical attention immediately if you develop:
- Sudden, severe abdominal or back pain
- Collapse or fainting
- Signs of shock
At Sharkawy Vascular Clinic, your care focuses on early detection, personalised surveillance, and evidence-based treatment to prevent rupture and protect your long-term health.

Stroke & Carotid Artery Disease
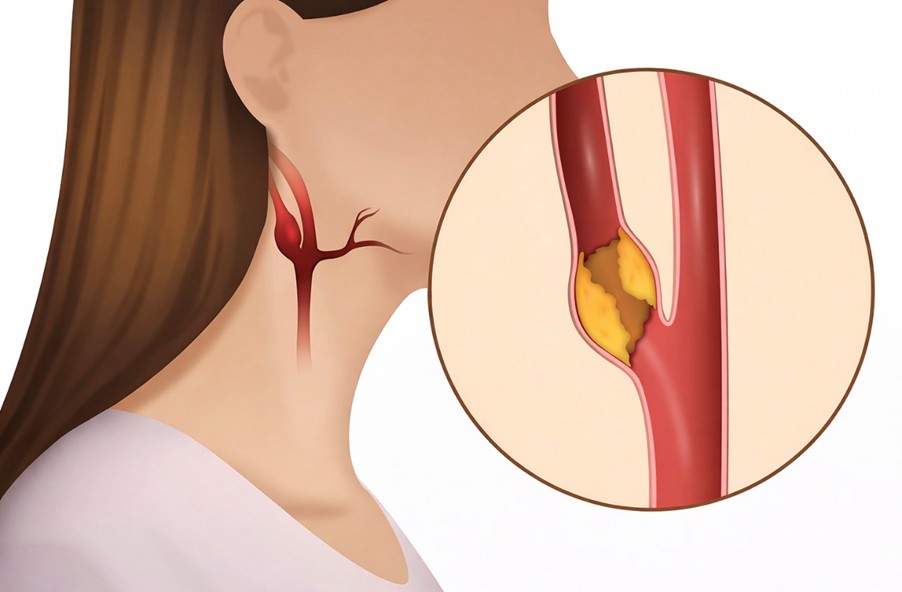
Carotid artery disease develops when fatty deposits (plaques) build up inside the arteries in your neck that supply blood to your brain. These arteries are called the carotid arteries.
When they become narrowed or blocked, your risk of stroke increases significantly.
A stroke is a medical emergency. It happens when part of your brain loses its blood supply. Without oxygen, brain cells begin to die within minutes, which can lead to permanent disability or death.
Carotid artery disease usually develops slowly. In many cases, the first warning sign may be a transient ischaemic attack (TIA) or a stroke.
A TIA is a temporary interruption of blood flow to your brain. Symptoms resolve completely, but it is a serious warning that you are at high risk of a full stroke.
Symptoms
In the early stages, you may have no symptoms at all. Symptoms usually appear when blood flow to your brain becomes critically reduced.
Signs of a stroke or TIA include:
- Sudden numbness or weakness in your face, arm or leg — often on one side.
- Sudden difficulty speaking or understanding speech.
- Sudden loss of vision in one or both eyes.
- Sudden dizziness, unsteadiness or loss of balance.
- Sudden severe headache with no obvious cause.
When to Seek Medical Help
If you develop any symptoms of a stroke — even if they last only a few minutes — seek emergency medical care immediately.
Do not ignore temporary symptoms. A TIA is a warning sign that you are at high risk of a major stroke.
If you have risk factors for carotid artery disease, you should consider vascular assessment even if you feel well. Early detection significantly reduces your stroke risk.
Causes
Carotid artery disease is caused by atherosclerosis — the gradual build-up of cholesterol, fat, and inflammatory cells inside your artery walls.
As plaque accumulates:
- Your carotid arteries become narrowed.
- Blood flow to your brain is reduced.
- Oxygen and nutrients cannot reach brain tissue adequately.
Risk Factors
You are at higher risk if you:
- Have high blood pressure.
- Smoke or use tobacco.
- Have diabetes.
- Have high cholesterol or high triglycerides.
- Have a family history of atherosclerosis or heart disease.
- Are older.
- Are overweight or obese.
- Have sleep apnoea.
- Do not exercise regularly.
Many of these risk factors are treatable. Controlling them significantly reduces your stroke risk.
How Carotid Artery Disease Causes Stroke
Carotid artery disease is responsible for approximately 10% of strokes. Stroke can occur in several ways:
1. Severely Reduced Blood Flow
Your artery may become so narrowed that insufficient blood reaches part of your brain.
2. Plaque Rupture
A fragment of plaque can break off and travel to smaller brain arteries, blocking blood flow.
3. Blood Clot Formation
Plaques can crack, triggering clot formation. A clot may grow large enough to block the artery or travel to the brain.
All three mechanisms can suddenly stop blood supply to part of your brain.
Protecting Yourself
Early diagnosis and treatment can prevent stroke. Management may include:
- Strict blood pressure control
- Cholesterol-lowering medication
- Antiplatelet therapy
- Lifestyle modification
- Carotid endarterectomy or carotid stenting in selected patients
If you have experienced a TIA, stroke symptoms, or have multiple vascular risk factors, specialist assessment is essential.
Diagnosis of Carotid Artery Disease
Your assessment usually begins with a detailed medical history and physical examination.
During the examination, your neck will be checked with a stethoscope to listen for a “bruit” — a whooshing sound caused by turbulent blood flow in a narrowed carotid artery.
You may also undergo a brief neurological assessment to check your:
- Strength
- Speech
- Memory
- Coordination
These tests help determine whether your brain circulation has already been affected.
Imaging Tests
To confirm the diagnosis and assess severity, you may need imaging tests.
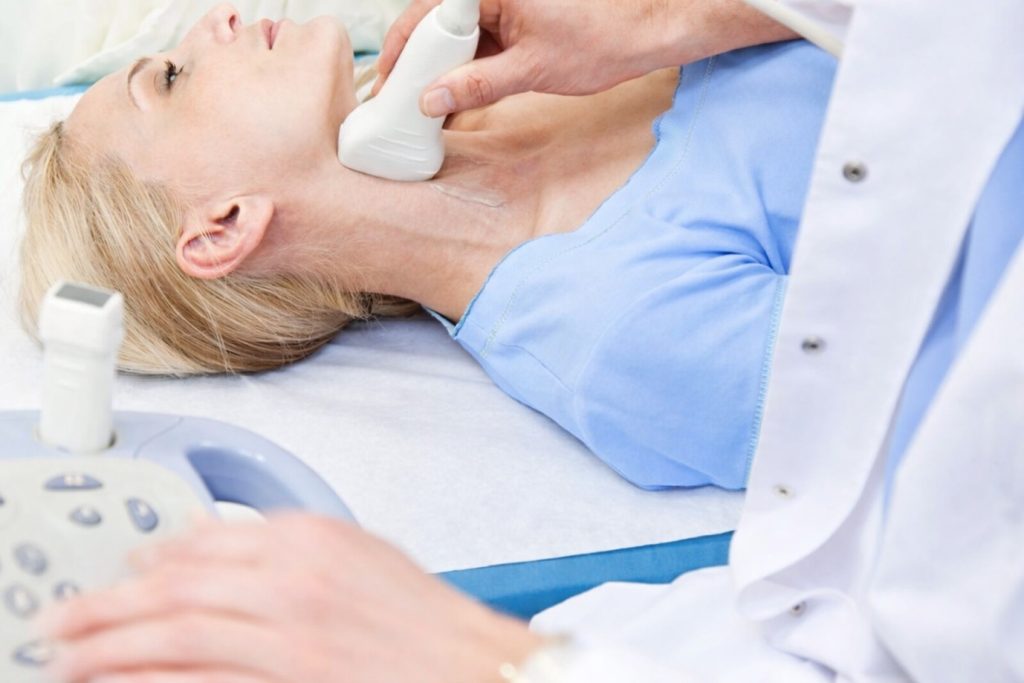
Carotid Ultrasound (Doppler Scan)
This is usually the first test performed. It measures blood flow and identifies narrowing within your carotid arteries. It is painless and non-invasive.
CT Scan or MRI
These scans can show whether you have already had a stroke or silent brain injury.
CT Angiography (CTA) or MR Angiography (MRA)
These specialised scans provide detailed images of your carotid arteries and brain circulation. A contrast dye is injected into a vein to make the arteries clearly visible.
Treatment of Carotid Artery Disease
The main aim of treatment is to prevent stroke.
Your treatment plan depends on:
- How severe the narrowing is
- Whether you have had symptoms (TIA or stroke)
- Your age and general health
If Your Narrowing is Mild to Moderate
Treatment usually focuses on reducing further plaque build-up and lowering stroke risk.
You may be advised to:
- Stop smoking
- Lose excess weight
- Follow a heart-healthy diet
- Reduce salt intake
- Exercise regularly
Medications are often prescribed, including:
- Blood pressure treatment
- Cholesterol-lowering therapy (statins)
- Antiplatelet medication such as aspirin or clopidogrel to reduce clot formation
If Your Narrowing is Severe or You Have Had a TIA or Stroke
Intervention may be recommended to remove or treat the blockage.
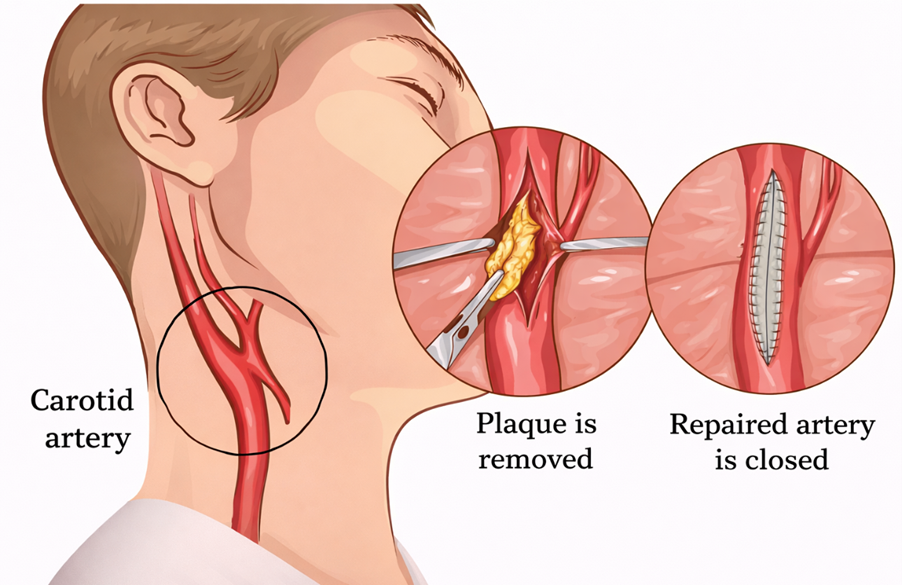
Carotid Endarterectomy
This is the most established surgical treatment for significant carotid narrowing.
An incision is made at the front of your neck. The carotid artery is opened, the plaque is removed, and the artery is repaired using stitches or a patch.
This procedure directly removes the blockage and restores blood flow to your brain.
Carotid Angioplasty and Stenting
This minimally invasive procedure may be recommended if:
- You have medical conditions that make you unfit for the gold standard endarterectomy operation.
Why Early Assessment Matters
Carotid artery disease can remain silent until a stroke occurs. Identifying and treating significant narrowing early can dramatically reduce your stroke risk.
If you have experienced a TIA, stroke symptoms, or have multiple cardiovascular risk factors, specialist vascular assessment is strongly recommended.
Prevention is far safer than emergency treatment.

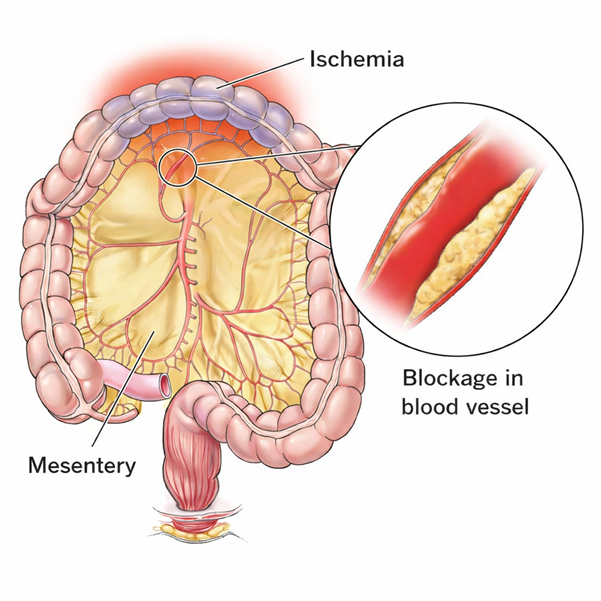
Mesenteric Ischaemia
(Reduced blood supply to your bowel)
Mesenteric ischaemia occurs when the arteries supplying your small intestine become narrowed or blocked, reducing blood flow. If untreated, the reduced circulation can permanently damage your intestine.
When this problem develops gradually over time, it is called chronic mesenteric ischaemia. It is usually caused by a build-up of fatty deposits (atherosclerosis) within the mesenteric arteries (arteries that supply your bowel)
If left untreated, the chronic form can suddenly worsen and become an emergency (acute mesenteric ischaemia). It can also lead to severe weight loss and malnutrition.
Symptoms You Should Not Ignore
You may experience:
- Abdominal pain starting about30 minutes after eating.
- Pain that gradually worsens over the next hour.
- Progressivefear of eating.
- Unintentional weight loss.
If you develop sudden, severe, persistent abdominal pain, seek urgent emergency care.
If you notice repeated pain after meals, you should arrange specialist vascular assessment without delay.
Why It Happens
Your small bowel relies on three main arteries for blood supply. When these arteries narrow due to plaque build-up, blood flow becomes insufficient — particularly after meals, when your bowel needs more oxygen.
Chronic mesenteric ischaemia is most often caused by:
- Atherosclerosis (fatty plaque narrowing the arteries)
Acute mesenteric ischaemia may occur due to:
- A blood clot (often originating from the heart)
- Sudden blockage of a mesenteric artery (artery supply your bowel)
Risk Factors
You are at higher risk if you have:
- Type 2 diabetes
- High blood pressure
- High cholesterol
- Smoking history
- Obesity
- Known vascular disease
- Atrial fibrillation
- Heart failure
Potential Complications
Without treatment, you may develop:
- Severe weight loss
- Malnutrition
- Acute-on-chronic mesenteric ischaemia (a life-threatening emergency)
Early diagnosis prevents irreversible bowel damage.
When to Seek Specialist Review
If you have:
- Post-meal abdominal pain
- Unexplained weight loss
- Known vascular disease with new abdominal symptoms
You should not delay assessment. Chronic mesenteric ischaemia is treatable — but timing is critical.
Early intervention can restore blood flow, relieve pain, and prevent life-threatening complications.
Diagnosis of Chronic Mesenteric Ischaemia
If you develop abdominal pain after eating and begin limiting your food intake or losing weight unintentionally, this raises concern for chronic mesenteric ischaemia.
The diagnosis is confirmed by demonstrating narrowing or blockage in the main arteries supplying your small bowel.
At Sharkawy Vascular Clinic, you will undergo a structured vascular assessment and advanced imaging techniques to accurately define the severity and anatomical pattern of disease.
Investigations You May Require
1. Doppler Ultrasound
This non-invasive test assesses blood flow velocity in the mesenteric arteries. It is useful for:
- Initial screening
- Follow-up after treatment.
2. CT Angiography (CTA) or MR Angiography (MRA)
These specialised scans provide detailed images of your bowel arteries.
A contrast dye is injected into a vein to make the arteries clearly visible.
All imaging is carefully reviewed to determine:
- Degree of stenosis
- Number of vessels involved
- Suitability for key-hole versus open intervention
When to Seek Specialist Assessment
Arrange urgent review if you have:
- Recurrent abdominal pain after eating
- Unexplained weight loss
- Known vascular disease with new abdominal symptoms
Chronic mesenteric ischaemia is treatable. Early specialist intervention prevents progression to acute intestinal infarction and avoids irreversible bowel damage.
Treatment of Mesenteric Ischaemia
At Sharkawy Vascular Clinic, treatment options include:
1. Endovascular Revascularisation (Minimally Invasive)
- Balloon angioplasty to open the narrowed artery
- Stent placement to maintain patency
- Performed through a small arterial puncture
This approach offers:
- Shorter recovery time
- Reduced surgical trauma
- Effective symptom relief in appropriate cases
2. Open Surgical Revascularisation
For complex disease, open bypass surgery may provide more durable long-term results.
This involves:
- Creating a bypass graft to restore blood flow
- Direct arterial reconstruction when required
My Approach to Your Care
As a Consultant Vascular & Endovascular Surgeon, I provide:
- Comprehensive diagnostic evaluation
- Individualised treatment planning
- Expertise in both open and advanced endovascular techniques
- Care tailored to complex multi-vessel mesenteric disease
You will receive a treatment strategy based on your anatomy, symptom severity, co-morbidities, and long-term durability.

Peripheral Arterial Disease (blocked arteries)
Lorem ipsum dolor sit amet, pri id summo detracto, cu usu magna omnes persecuti. Alia postea vix id, ne est dicta simul definiebas, nec ex agam dolor summ.
Get in contact
HAVE A QUESTION ABOUT THIS?

